In many radiological and orthopedic workflows, precise calibration of an X-ray image is an essential prerequisite for digital preoperative planning. Without a reference object of known size, the relative dimensions within the image can only be assessed with limited reliability, as every radiograph is subject to a certain degree of magnification. This is precisely why digital planning systems use calibration markers that are visible on the X-ray image and have a clearly defined diameter.
In everyday clinical practice, however, an effective solution does not necessarily have to be expensive, complex, or dependent on specialized external products. A particularly practical approach is the use of a revised femoral head with a known diameter of 28 mm as a calibration marker. This defined size is the decisive factor for radiological calibration. Scientific publications explicitly describe the use of a 28 mm cobalt-chromium femoral head as a viable alternative when a standardized calibration marker is not available.
Why a 28 mm femoral head?
A revised prosthetic femoral head offers several clear advantages over improvised everyday objects: it is radiopaque, dimensionally stable, spherical, and has a known, reproducible diameter. These are exactly the characteristics required for a reliable calibration marker. While unsuitable or incorrectly positioned external markers may distort measurements, an object with a defined size can serve as a dependable reference — provided it is positioned at the correct anatomical level. Ultimately, the quality of calibration depends not only on the marker itself, but above all on its position relative to the joint or bone plane.
The pragmatic clinical approach
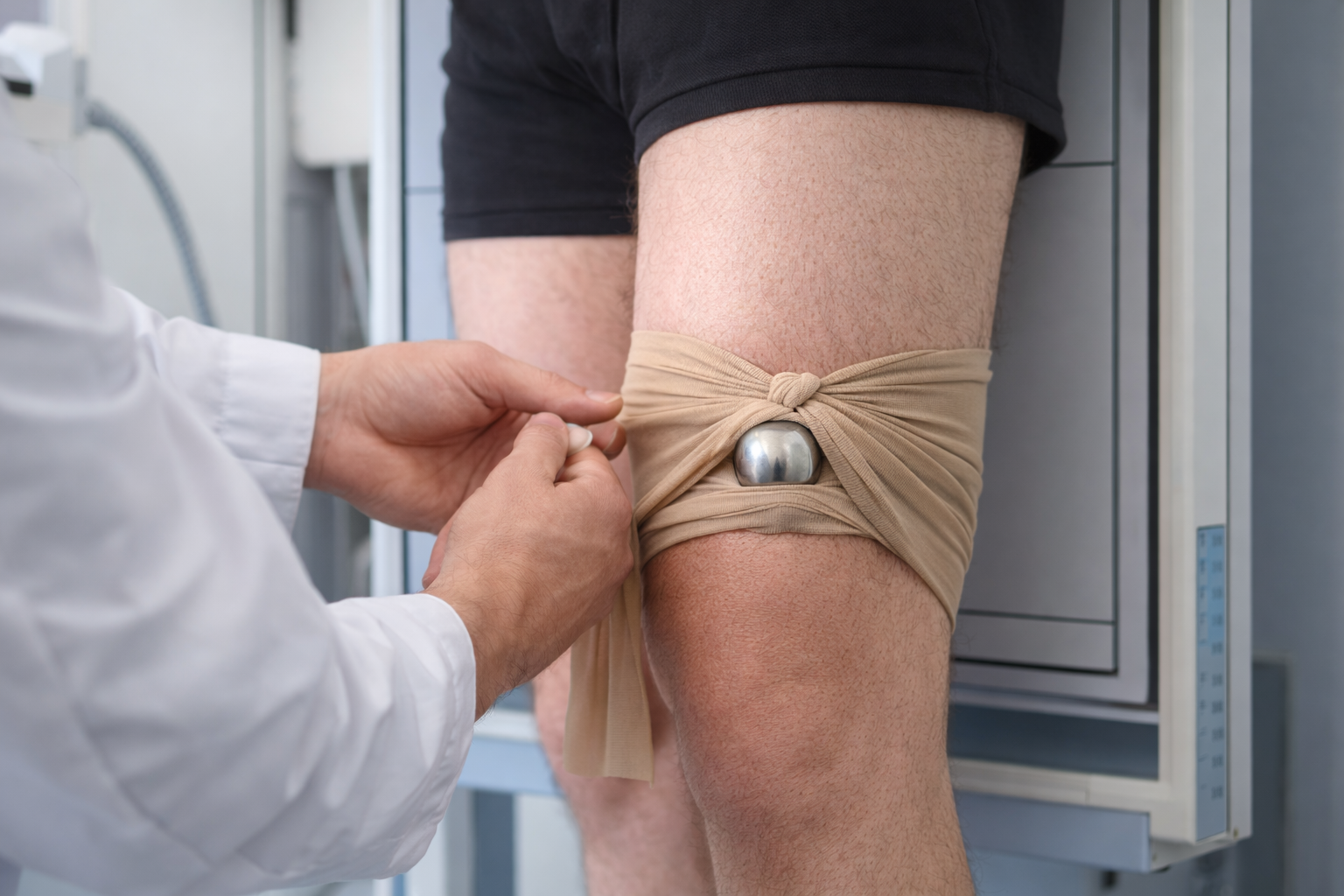
A simple yet surprisingly practical option is to place the 28 mm femoral head inside elastic pantyhose or a similarly flexible and secure holding material. This allows the sphere to be positioned during image acquisition as close as possible to the anatomically relevant plane. In clinical practice, it may be fixed, for example, near the knee joint or the affected extremity, while still allowing precise adjustment within the material until the desired level is reached.
The actual benefit of this approach is easy to understand:
It is not merely the presence of any sphere in the X-ray field that improves planning accuracy, but the presence of a sphere with a known diameter that is positioned as close as possible to the relevant bone or joint plane. This is where the real value for subsequent digital planning arises. The literature clearly shows that incorrect positioning of external markers can significantly compromise accuracy, whereas calibration using objects of known size at the correct plane is considerably more reliable.
What makes this approach valuable
The main advantage of this method lies not only in its simplicity, but also in its practicality. In many hospitals, revised prosthetic components are already known, available, or accessible. Instead of maintaining additional specialized markers for each department, an existing sphere of known size — provided it has been internally approved — can represent a highly economical and practical solution. This reduces procurement effort, lowers additional costs, and simplifies implementation without losing sight of the central principle of calibration: a clearly defined reference size positioned at the correct anatomical plane.
It is not the cost that matters — it is the correct positioning.
This is where clinical workflows are often unnecessarily overcomplicated. Not every commercial marker system is automatically superior. Studies have shown that conventional external markers may also be prone to error under everyday clinical conditions if they are not positioned precisely at the level of the hip center or target region. The critical factor is therefore not the price of the product, but its correct placement. A simple marker of defined size can be clinically more useful than an expensive system that is applied incorrectly.
An important note for radiology and operating room environments
As pragmatic as this approach may be, internal hygiene regulations, reprocessing requirements, material approvals, and institutional procedures must always be observed in everyday hospital practice. A prosthetic femoral head may only be used as a calibration marker if this is properly regulated from an organizational, hygienic, and procedural perspective. The practical value of this idea lies not in uncontrolled improvisation, but in standardized, traceable, and approved application.
Conclusion
X-ray calibration markers do not necessarily have to be expensive in order to reliably serve their purpose. For digital preoperative planning, the essential requirement is that the image contains a radiologically visible object of known size and that this object is positioned as close as possible to the relevant anatomical region.
The marker should be placed in the correct anatomical plane. A revised 28 mm femoral head can be an exceptionally practical, economical, and intelligent solution for this purpose — provided it is used correctly and in accordance with internal guidelines.
The collaboration between radiology, surgery, and medical staff demonstrates that good clinical processes do not always result from higher costs, but often from intelligent, standardized, and practical solutions.

